Innovating Payment Integrity, One Solution at a Time
Technology.
Precision.
Results.
360 Health Systems is a tech-first partner delivering a portfolio of advanced solutions designed to improve payment accuracy and audit efficiency. From overpayment oversight to DRG grouping and pricing, our innovations help healthcare organizations streamline operations, safeguard revenue, and achieve lasting financial integrity.

Engineered for Precision in Payment Integrity
Built by 360 Health Systems, PORA is the flagship platform in our solutions portfolio , combining automation, analytics, and audit intelligence to help organizations detect overpayments faster, recover revenue more effectively, and oversee audit processes from start to finish.
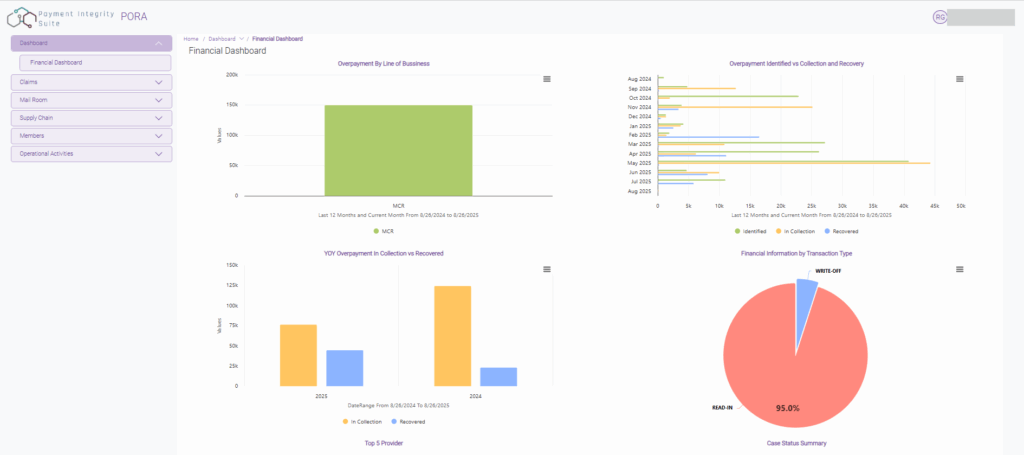
Full-Scope Overpayment Management
Support across the full claims lifecycle, from identification through resolution.
Built-In Algorithms
Harness advanced algorithms, machine learning, and intelligent analytics to pinpoint overpayments faster, prioritize high-value cases, and improve recovery rates.
Seamless Integration
Our API architecture enables scalable and secure functionality, ensuring your teams can start benefiting from advanced overpayment oversight tools right away. Built with state-of-the-art security standards, our solutions deploy quickly and adapt to your operational environment without disruption.

Why 360 Health Systems?
360 Health Systems is more than a product company—we are a technology-first partner dedicated to advancing payment integrity. Driven by the principle of human intelligence driving innovation, we leverage our expertise and technology to deliver solutions that enhance efficiency and foster long-term value. With PORA as our flagship and a growing portfolio that includes DRG Grouping & Pricing and other intelligent solutions, we are committed to helping healthcare organizations achieve sustainable results, minimize operational friction, and prepare for the challenges ahead.
- Innovation Roadmap – Ongoing research and development that expands beyond PORA into next-generation payment integrity solutions.
- Trusted Expertise – A team with deep industry experience in payment integrity, audit, and healthcare compliance.
- Proven Outcomes – Demonstrated impact on overpayment detection, revenue recovery, and audit efficiency.
- Security First – State-of-the-art infrastructure designed to exceed healthcare data protection standards.
- Long-Term Partnership – A commitment to supporting organizations not just today, but as the industry evolves.
now and i absolutely love it”
Ready to Transform Your Payment Integrity?
Schedule a demo to see how 360 Health Systems can help you recover lost revenue and reduce financial waste.

